Spasticity offers its own set of challenges for someone with MS. However, the best—and simplest—message about spasticity and MS is that there are ways of controlling it. Because it needs individual management, you should seek advice and assessment early. You can call on your GP, neurologist and/or hospital-based services. We can also help. Regional MS Societies have trained and experienced Community Support Staff who provide a wide variety of services and practical support to people with MS, their carers and families, as well as advice on all matters concerning MS.
Within the body’s central nervous system there is a complex interactive process that controls the contraction and relaxation of muscles. Nerve pathways direct messages between the brain and muscles to produce the movement that you want.
For example, when we make a fist, there is simultaneously:
However, MS damages the nervous system and this interferes with the coordination or movement of muscles, particularly with getting them to relax. Muscles affected by spasticity generally feel stiff or cramped, and can lock a joint into position until the muscle tension is reduced by fatigue or by stretch techniques. The level of spasticity may vary from a mild increase in muscle stiffness (which can be relatively easy to control), to sudden strong spasms that contract muscles in rigid positions (which can be difficult to overcome). The strength of the reaction can depend on the damage to the central nervous system, i.e. the severity of the MS. The more nerve fibres that are affected, the more easily triggered and harder to overcome spasticity becomes.
Aside from the neurological damage, other common causes of a spastic reaction for people with MS are:
The next few sections suggest some approaches for preventing and managing spasticity, and they can be used regardless of how the reactions were caused. It is always recommended to consult a professional, eg. physiotherapist, to review and advise the best options for your individual needs.
Hypertonic or spastic muscles go into spasm in patterns dictated by the strength of the muscle groups to which they belong:
Lower Limbs
In this muscle group, the most common position for spastic muscles is with the hips and knees pulled straight, legs pulled together and foot pointed down. However, in a few cases, the opposite patterns may co-exist or predominate and the legs may draw up into a flexor pattern—hips, knees and feet pulled up towards the torso.
Upper Limbs
The common position for spastic muscles is with the elbows, wrist, fingers bent and the arm pulled across the body, similar to when you eat with your hands. Again, in some people the opposite pattern may predominate and the elbow may be pulled straight.
Torso
In the torso, the back muscles that lie on either side of the spine may also spasm. This produces a very strong pattern that arches the back and neck and very often triggers a straightening response in the legs. This response can make transfers from a chair to the toilet, car or bed very difficult. Stretching your arms over your head will often trigger the back muscles into a spasm. These spastic reactions can be frustrating, and interfere with your day-to-day activities. However, there are times when the presence of spasticity can be beneficial. For example, it can assist positional changes in bed. A sharp pull on a bed bar can induce a flexor spasm—this raises the knees, and in turn allows you to turn onto your side, easing pressure points on back, buttocks and heels. A later push on the bar will trigger an extensor spasm—this allows you to return to your back. So, whilst spasticity can be frustrating, it can also provide extra help with your movements.
Controlling Mild Spasticity
It is important to address problems with spasticity, as it can eventually lead to muscle shortening as well as posture and joint troubles. The best management methods are concerned with prevention, using stress management and gentle exercise. Other tools include physical therapy aids and medication. You should involve your family, carer and health professionals in your treatment, as a team approach can provide both physical and motivational support.
Stress management
Mental and emotional stress can increase muscle tension and contribute to spasticity, so it is important to include stress management in your programme of spasticity control. Some good ideas for managing stress include:
Your local MS Society may provide some of these services or be able to recommend and refer to other services in the community. Also, it is crucially important that you contact your Regional MS Community Staff, your GP, or a psychologist if stress from family or financial pressures, or the challenges of living with MS, become overwhelming. Help is available.
Spasticity may be triggered by contraction of only one muscle, but relaxing the whole muscle group by slow, sustained stretching will ease the tightness. It is also good to use deliberate body positioning to prevent spasticity. There are other activities that can help relax tight muscles, such as horse riding, swimming, massage and acupuncture. Always talk to your doctor or a physiotherapist before starting any exercise programme. Don’t overdo it when exercising, particularly at first. One of the symptoms of MS is decreased endurance with early fatigue. Usually 3-5 repetitions of a given exercise are an effective number. Gradually increase the number as you feel able. Progress may be slow, but persevere—try to set yourself realistic exercise goals. Be prepared to rest after your exercise time.
Note: Some health professionals suggest ice packs or splinting for spasticity. However, you should be very careful as they can increase muscle tension, and the ice packs can damage your skin.
Stretching
Before starting any strengthening exercises, you should do some stretching:
Stretching on your own
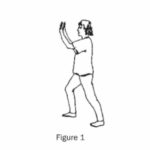
(a) Standing against a wall or chair, place one foot behind the other. With your front knee bent slightly, keep your back leg straight and your heel down. Lean your hips forward until you feel a stretch in your calf (Figure 1). Repeat with the other leg.
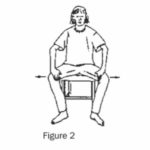
(b) Sit on the front of a chair or bench. Place your legs fairly wide apart, with your knees bent and feet flat on the floor, pointing in the same direction as your knees. Place your hands against your lower thighs near the knees. Lean gently forward, while pushing your thighs apart (Figure 2).
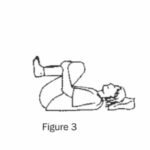
(c) Lying on your back, lift both knees to your chest. Wrap your arms around your legs just below your knees. Pull your knees to your chest while pushing your tailbone towards the ground (Figure 3).
Stretching with a helper
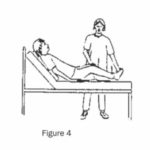
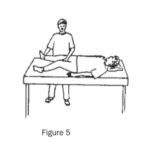
(d) Lie on your back while a helper bends your knee towards the body, making sure your knee does not turn outwards throughout the movement. Then move the leg back (Figure 4). Repeat with the other leg. (e) With legs together and straight, have a helper move one leg apart, then back to the starting position (Figure 5). Repeat with the other leg.
Strengthening
Strengthening exercises
You should consult with your doctor and physiotherapist to ensure these exercises are within your physical capabilities and can be performed safely. Take care not to push yourself too hard and pace yourself to avoid fatigue. These exercises are suitable whether you are mobile or spend much of the day sitting. They are best performed once the muscles have warmed up and before any fatigue sets in, i.e. mid-morning.
Repeat each exercise five times to begin with and gradually increase the number, as you feel able:
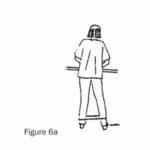
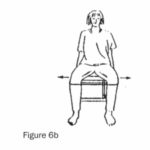
(a) Sit, stand or lie with a one metre loop of wide elastic around knees (or ankles for a stronger exercise). Pull your legs apart against the resistance (Figures 6a and 6b).
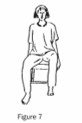
(b) Sit with legs apart. Lift toes, then whole foot off the ground, one leg at a time. If this movement is very weak, give yourself some assistance with your hands. Try to hold your back straight and your stomach in. (Figure 7.)
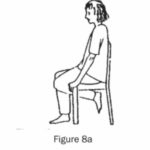
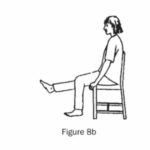
(c) Sit with knees apart. Try to gently kick the underside of the seat, then straighten your knee out. (Figures 8a and 8b.)
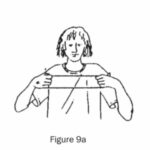
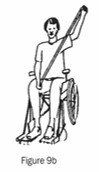
(d) Hold the elastic band and use it like a chest expander. (Figures 9a and 9b.) Keep your knees apart with a pillow, as this will reduce the spastic reaction of stretching above your head.
Some suggestions for comfortable positions throughout the day
Comfortable positions that oppose common spasticity patterns, and that can be held for one hour or more, can be beneficial.
These include:

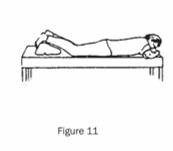
Some adaptive devices are available to assist your gait, posture and movements. A consultation with a physiotherapist, or an occupational therapist can be useful. For example, they may suggest orthotics – which are lightweight shoe inserts used to position a spastic foot correctly. Additionally, orthotics can reduce fatigue and increase walking stability.
There are several drugs that can be valuable in controlling spasticity, but these drugs affect all the muscles of the body, not just the tight ones. The results can be increased weakness and fatigue. Therefore, reducing the spasticity must be traded against other physical weakness and increasing your problems with standing, transferring from bed, chair, toilet, etc. Your GP or neurologist will be able to discuss your options in appropriate detail.
In cases where severe spasticity develops, or untreated spasticity has caused permanent muscle shortening, more aggressive intervention may be needed.
Chemical nerve blocks
Botulinum Toxin (Botox) can be used for temporary management of severe spasticity in an isolated area. A Baclofen pump can also be considered. This is a small disc inserted into the spinal column and programmed to release medication. After the intial operation, it is refilled by injection. Phenol gives a long lasting reduction in tension in specific muscles. But it is no longer the preferred option, given the effectiveness of the above two chemicals.
Surgery
Surgery may be necessary in severe cases – especially if the muscles have shortened and caused contracted joints. Your doctor will discuss this solution with you.
For more information please view our MSNZ Information Series booklet: Multiple Sclerosis and Spasticity